Autism
ASD Prevalence
Autism Spectrum Disorder (ASD), also simply called Autism, is a marked by differences in communication, play, sensory processing, interests, and behaviour. Traditional thinking held that ASD was rare in people with Down syndrome (DS) or symptoms could be accounted for by cognitive abilities, but that is far from the case. In fact, it is estimated that ASD in individuals with DS is 10-25 times more common than in the typical population (1.7%), 16-42% of individuals with DS meet the criteria for ASD. At the Down Syndrome Resource Foundation, our prevalence rate is in line with these studies, with approximately 12% of our students having a dual diagnosis.
Diagnosis
Unlike DS, which is diagnosed through a blood test, ASD is a subjective diagnosis based upon observed behaviours and social communication patterns. Unfortunately, the research on ASD and DS is limited, which makes understanding this dual diagnosis difficult, for families and health care professionals. ASD diagnosis often comes much later in people with DS than it would for other children, especially for girls. In one study of subjects with a dual diagnosis, the mean age of ASD diagnosis was 14.4 years – even though, as with other children, autistic symptoms were present much earlier in life (before the age of three). Reasons for these delays could be due to lack of education, awareness and understanding or the fact that development is slower in DS, thus symptoms may not be as obvious until later.
DS and Autistic Learning Profiles
Students with a dual diagnosis of ASD and DS have a distinct profile that differs from others with a single diagnosis of ASD or DS. Below is what we currently understand about the unique developmental profile that is DS and ASD.
Research has found that students with ASD and DS compared to students with a single diagnosis of DS:
- Use less symbolic communication and conventional gestures (for example, waving for “hi,” hands up to request “up” or pointing to say “look!”). Often, parents describe that they can understand what their child is communicating by reading their body movements (e.g. hand flapping, teeth grinding, leaving) and vocalizations. They report their child uses more nonsymbolic and unconventional gestures, such as pulling, pushing, reaching, or using your hands to do things for longer before they learn language.
- Need support in both understanding and expressing themselves or their expressive language (words they use) may be higher than their receptive language (words they understand). They may use scripting or process language in “chunks” rather than individual words. They may use echolalia (repeating things they hear) more often. When they repeat, it is often in the same rhythm and intonation. For example, if you ask your child, “Want a cookie?” they may say, “Want a cookie?” whenever they have snack, regardless of there being cookies there or not.
- Use less joint attention and back and forth imitation, they prefer to focus their attention on one thing at a time rather than shift their attention to various things. Parents often describe their child as “being in their own world.” They may get your attention when they need help or want something, but seldom to show something to you or look when you point to something.
- Less variety in facial expressions, some parents report it is difficult to read their child’s thoughts and feelings based on their facial expressions or they have certain ones for specific situations.
- Prefer cause and effect and sensory play as opposed to pretend play. Parents often report they may focus on part of a toy (e.g. spinning a wheel on a toy car) rather than using it as a whole (e.g. driving a toy car).
- Display strong interest in objects, letters, or numbers. Students may show fascination with certain objects or when learning to read, may decode before what is expected for their age (Hyperlexia).
- Increased frequency and intensity of stimming, hyperactivity, challenging and self-injurious behaviours (e.g. biting, hitting) or sensory, feeding and sleep challenges. Often parents describe that their child is very particular and has strong emotional reactions or meltdowns to unforeseen changes, demands and sensory overload.
- Are more at risk of experiencing a developmental regression or plateau.
Research has found that students with ASD and DS compared to students with a single diagnosis of ASD:
- Gesture more frequently
- Show more interest in people and surroundings
- Are more likely to imitate others
- Are less impulsive
This diagram illustrates the characteristics we currently understand that are commonly associated with DS and ASD, highlighting the developmental differences in how our students learn, play, communicate, process sensory information, and socialize:
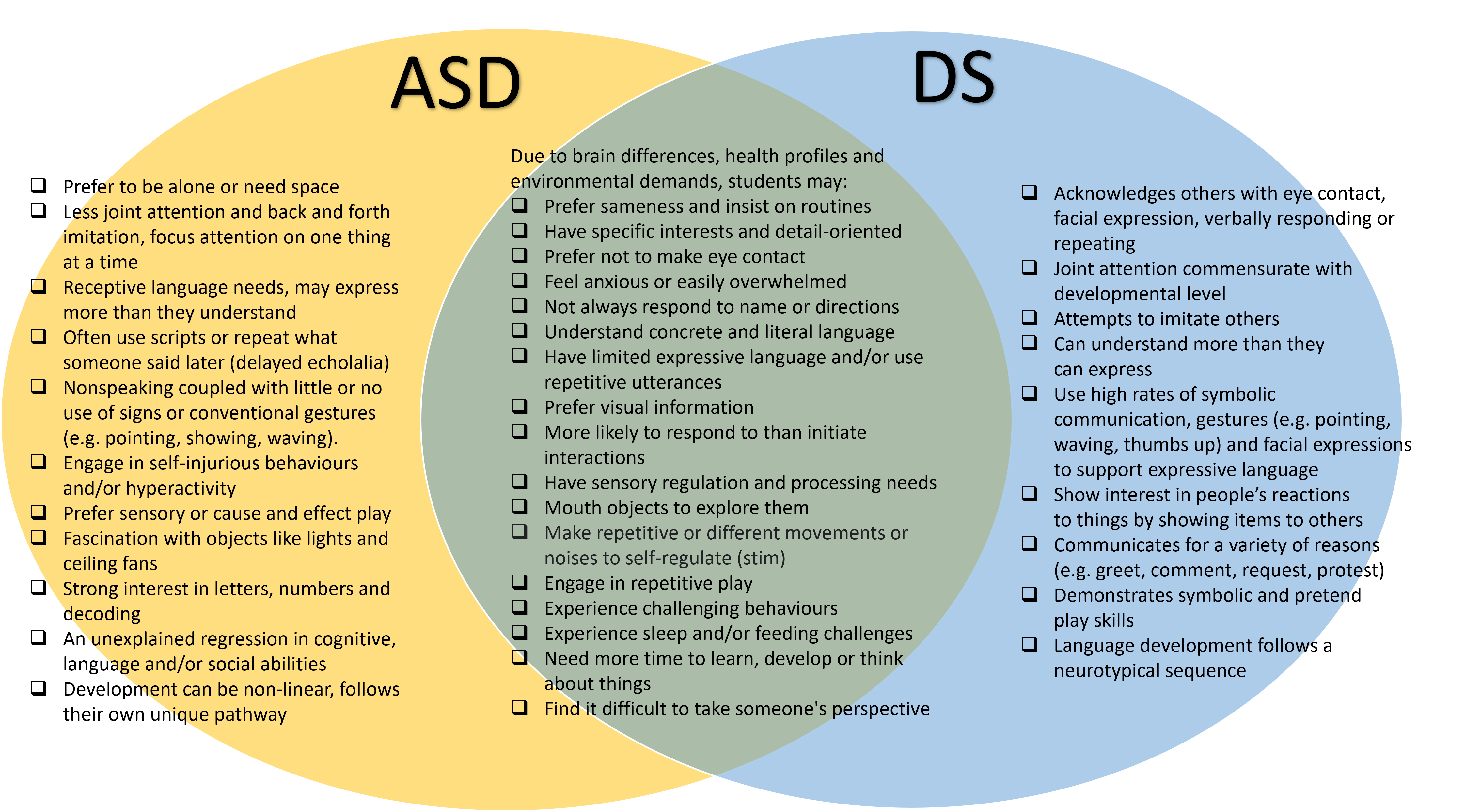
Despite there being a lot of overlapping characteristics, the more signs and symptoms that are present, the more likely it is that your child or student may be Autistic. The frequency, intensity and complexity of these characteristics should be considered. Autism is considered a spectrum because each autistic person is unique and varies in how much or how little they may display certain autistic traits. No two people with ASD and DS are alike, each experience symptoms in different ways. This website illustrates how the idea of a ‘spectrum’ can be thought of in relation to autism.
What to Do if You Suspect Your Child is Autistic
If you suspect your child or someone you know is autistic, the first step is to consult with one or more members of your professional support team, such as your pediatrician, speech therapist, or child psychologist. A team approach can help determine if the characteristics DS are best explained by the developmental profile associated with DS alone or the dual diagnosis of DS + ASD. If they share your observations, they can provide you with a referral for a formal assessment.
For many parents, adding another label (and another long series of assessments) is the last thing they want. However, an accurate diagnosis is important in fully understanding your how child learns, processes information, and communicates will help them get the best possible educational and vocational support. Having a diagnosis of ASD could inform medical decisions and can help us understand their unique needs that could be creating learning challenges. Label or no label – they are who they are, in all their strengths, challenges, and personality!
ASD and DS: A Parent’s Perspective
Everyone’s experience being a parent of an Autistic child with Down syndrome is different. According to a survey we did in 2020, some of our families reported the following after their child received a diagnosis: excitement, relief, and an increased understanding of their child, including their communication, sensory needs, and behaviours. They felt better supported and validated, having access to professionals, increased support at school and funding for materials, therapies, and community programs.
Other parents reported heightened stress, frustration, and feelings of isolation, that they do not fully fit into the Autism or DS community. By providing families with the following resources about dual diagnosis, we hope to increase our families’ ability to understand and advocate with their child and connect with others who share similar journeys.
DSRF Resources
Dual Diagnosis: Down Syndrome + Autism (Down Syndrome Academy online learning course)
The LowDOWN Podcast – Dual Diagnosis: The Down Syndrome-Autism Connection (Oct. 28, 2020)
The LowDOWN Podcast – It’s Complicated: When Down Syndrome Meets Autism (Nov. 1, 2023)
Putting the Pieces Together: The Down Syndrome-Autism Intersection
Other Resources
Start Here: A Guide for Parents of Autistic Kids
Family Resources – Autism Navigator
The Down Syndrome – Autism Connection
A Closer Look at Social Communication Difficulties of Children with Autism Spectrum Disorder
“Tuning In” to Others: How Young Children Develop Theory of Mind
A List of Apps for Social Skills and Autism Spectrum Disorders
References
Capone, G.T. (2001) Down syndrome and autistic spectrum disorder: a look at what we know. www.dsmig.org.uk Down’s Syndrome Association Newsletter
Cook A, Quinn ED, Rowland C. Exploring Expressive Communication Skills in a Cross-Sectional Sample of Individuals With a Dual Diagnosis of Autism Spectrum Disorder and Down Syndrome. Am J Intellect Dev Disabil. 2021 Mar 1;126(2):97-113. doi: 10.1352/1944-7558-126.2.97. PMID: 33651892; PMCID: PMC8552670.
Channell, M. M., Phillips, B. A., Loveall, S. J., Conners, F. A., Bussanich, P. M., & Klinger, L. G. (2015). Patterns of autism spectrum symptomatology in individuals with Down syndrome without comorbid autism spectrum disorder. Journal of neurodevelopmental disorders, 7(1), 5. https://doi.org/10.1186/1866-1955-7-5
DiGuiseppi, C., Hepburn, S., Davis, J. M., Fidler, D. J., Hartway, S., Lee, N. R., Miller, L., Ruttenber, M., & Robinson, C. (2010). Screening for autism spectrum disorders in children with Down syndrome: population prevalence and screening test characteristics. Journal of developmental and behavioral pediatrics : JDBP, 31(3), 181–191. https://doi.org/10.1097/DBP.0b013e3181d5aa6d
Godfrey M, Hepburn S, Fidler DJ, Tapera T, Zhang F, Rosenberg CR, Raitano Lee N. Autism spectrum disorder (ASD) symptom profiles of children with comorbid Down syndrome (DS) and ASD: A comparison with children with DS-only and ASD-only. Res Dev Disabil. 2019 Jun;89:83-93. doi: 10.1016/j.ridd.2019.03.003. Epub 2019 Apr 6. PMID: 30959431.
lasin, R.. (2008). Age at Regression in Children With Autism With and Without Down Syndrome. Aap Grand Rounds. 20. 33-34. 10.1542/gr.20-3-33.
Lorang, E., Sterling, A., & Expressive Language Consortium (2017). The impact of autism spectrum disorder symptoms on gesture use in fragile X syndrome and Down syndrome. Autism & developmental language impairments, 2, 10.1177/2396941517745673. https://doi.org/10.1177/239694151774567
Moss J, Richards C, Nelson L, Oliver C. Prevalence of autism spectrum disorder symptomatology and related behavioural characteristics in individuals with Down syndrome. Autism. 2013 Jul;17(4):390-404. doi: 10.1177/1362361312442790. Epub 2012 May 15. PMID: 22589453.
Versaci TM, Mattie LJ, Imming LJ. Down Syndrome and Autism Spectrum Disorder Dual Diagnosis: Important Considerations for Speech-Language Pathologists. Am J Speech Lang Pathol. 2021 Jan 27;30(1):34-46. doi: 10.1044/2020_AJSLP-20-00050. Epub 2020 Dec 14. PMID: 33316160.
